History and Development of Neuroendovascular Therapy
Society
The organization of Japan’s society for neuroendovascular therapy began in 1982, when the late Professor Naoki Kageyama of Nagoya University Neurosurgery foresaw the potential of this treatment—already emerging in Europe—and launched the “Japanese Study Group of Intravascular Surgery.”
Makoto Negoro, who participated in the Workshop of Interventional Neuroradiology (WIN)—the Val d’Isère meeting, the predecessor of today’s World Federation of Interventional and Therapeutic Neuroradiology (WFITN)—served as secretariat.
In Japan, physicians including Katsuya Goto, Kazuro Taki, and Akira Takahashi had independently begun treatment in various regions, but joined this study group in response to Kageyama’s call.
The first meeting was held on December 10, 1982, at the Aichi Prefectural Industrial Trade Hall in Nagoya, with 21 presentations and roughly 200 participants. Meetings from the second (1983) through the fifth were held biennially in Nagoya. The first three were chaired by Naoki Kageyama, the fourth by Haruhiko Kikuchi, and the fifth by Kazuo Takeuchi. From the sixth meeting in 1990 (chaired by Keizo Matsumoto in Tokushima), meetings began rotating nationwide. The name changed from the “Japanese Study Group of Intravascular Neurosurgery” (from the 5th meeting, 1989) to the “Japanese Society for Neuroendovascular Therapy” from the 14th meeting (1998). The 11th meeting was held jointly with the 3rd Congress of the World Federation of Interventional and Therapeutic Neuroradiology in Kyoto, chaired by Kazuro Taki. By 2024, the society counted its 40th annual meeting. With the transition to a society, the English name changed from “Japanese Society of Intravascular Neurosurgery (JSIN)” to “Japanese Society for Neuroendovascular Therapy (JSNET).”
In 2000, a specialist certification system was established with 14 board members serving as supervising instructors, ensuring quality and lifelong education for neuroendovascular therapy. In 2001, 34 instructors were certified, and the first specialist examination began in 2002. By 2024, 24 examinations had been held.
In 2006, the society became a certified NPO, enabling specialist advertisement. Kazuro Taki of Kyoto University became the first president (2007–2012), reorganized the secretariat to Medical Tribune, founded the official journal “Journal of Neuroendovascular Therapy (JNET),” and joined the Japan Board of Medical Specialties. The second president (2012–2016), Akio Hyodo, moved the secretariat to the International Medical Information Center, secured annual meeting subsidies, enhanced the specialist system, initiated annual reports, and launched an English journal. The third president (2016–2021), Nobuyuki Sakai, established standards for new devices and proper use guidelines, contributing significantly to device introduction. In 2018, JSNET achieved long-awaited membership in the Japan Medical Association. In August 2022, immediately after his term, JSNET hosted the 16th WFITN Congress in Kyoto—the first since 2005. The fourth president (2021–2024), Shigeru Miyachi, transitioned the society to a general incorporated association, introduced a delegate system, and reformed the specialist examination process. The journal gained international recognition as an English-language journal, achieving PubMed indexing in 2024. Domestic device development also advanced. In 2024, Yuji Matsumaru became the fifth president, with further progress expected.
Past Presidents and Meeting Venues
| Conference | President | Venue |
|---|---|---|
| 1st Intravascular Surgery Study Group | Naoki Kageyama (Nagoya University) | Dec 10, 1982 – Aichi Prefectural Industrial Trade Hall |
| 2nd Intravascular Surgery Study Group | Naoki Kageyama (Nagoya University) | Dec 16, 1983 – Aichi Prefectural Industrial Trade Hall |
| 3rd Intravascular Surgery Study Group | Naoki Kageyama (Nagoya University) | Dec 7, 1985 – Aichi Prefectural Industrial Trade Hall |
| 4th Intravascular Surgery Study Group | Haruhiko Kikuchi (Kyoto University) | Dec 5, 1987 – Aichi Prefectural Industrial Trade Hall |
| 5th Japanese Study Group of Neuroendovascular Surgery | Kazuo Takeuchi (Kyorin University) | Nov 25, 1989 – Aichi Prefectural Industrial Trade Hall |
| 6th Japanese Study Group of Neuroendovascular Surgery | Keizo Matsumoto (Tokushima University) | Nov 12–13, 1990 – Tokushima Prefectural Culture Hall |
| 7th Japanese Study Group of Neuroendovascular Surgery | Shiro Waga (Mie University) | Nov 21–22, 1991 – Mie Prefecture Medical Association Hall |
| 8th Japanese Study Group of Neuroendovascular Surgery | Kintomo Takakura (University of Tokyo) | Nov 27–28, 1992 – Japan Firefighters Hall |
| 9th Japanese Study Group of Neuroendovascular Surgery | Takashi Yoshimoto (Tohoku University) | Nov 21–22, 1993 – Sendai International Center |
| 10th Japanese Study Group of Neuroendovascular Surgery | Ryuichi Tanaka (Niigata University) | Nov 24–25, 1994 – Niigata Civic Plaza |
| Joint International Conference on Neuroendovascular Therapy (WFITN) 11th Japanese Study Group of Neuroendovascular Surgery |
Honorary President: Haruhiko Kikuchi (Kyoto University) Kazuro Taki (Kyoto University) |
Nov 19–22, 1995 – Kyoto International Conference Center |
| 12th Japanese Study Group of Neuroendovascular Surgery | Makoto Negoro (Nagoya University) | Nov 20–21, 1996 – Nagoya International Conference Center |
| 13th Japanese Study Group of Neuroendovascular Surgery | Honorary President: Takashi Ohmoto Kazushi Kinugasa (Okayama University) |
Nov 20–21, 1997 – Hotel Granvia Okayama |
| 14th Japanese Society for Neuroendovascular Therapy | Makoto Sonobe (National Mito Hospital) | Nov 19–20, 1998 – Mito Civic Hall |
| 15th JSNET | Katsuya Goto (Iizuka Hospital) | Nov 17–19, 1999 – Fukuoka Sun Palace |
| 16th JSNET | Akira Takahashi (Tohoku University) | Nov 17–19, 2000 – Sendai International Center |
| 17th JSNET | Tetsuo Koike (Niigata City General Hospital) | Nov 21–23, 2001 – Niigata Prefectural Civic Center |
| 18th JSNET | Akio Hyodo (University of the Ryukyus) | Dec 4–6, 2002 – Okinawa Convention Center |
| 19th JSNET | Shigeru Nemoto (Toronomon Hospital) | Nov 17–19, 2003 – Pacifico Yokohama |
| 20th JSNET | Toshio Hyoshi (Nakamura Memorial Hospital) | Nov 17–19, 2004 – Sapporo Convention Center |
| 21st JSNET | Tomoaki Terada (Wakayama Medical University) | Nov 9–11, 2005 – Wakayama Prefectural Cultural Hall |
| 42nd Annual Meeting of JSNET | Yuichi Murayama (Tokyo Jikei University School of Medicine) | Nov 19–21, 2026 – Grand Prince Hotel New Takanawa |
Members
The number of members has continued to rise steadily, from 1,064 in 2000 to over 4,800 in 2024, making JSNET one of the largest academic societies.
Neuroendovascular therapy is fundamentally based on cerebral angiography. This was developed in 1927 by Egas Moniz and, almost simultaneously, in Japan by Professor Makoto Saito, the first professor of surgery at Nagoya University. As a result, neurosurgeons have traditionally taken the lead in performing cerebral angiography in Japan. The small number of neuroradiologists in Japan compared with overseas, and the extremely broad scope of practice covered by neurosurgeons—including radiation therapy and internal medicine—further explains why neurosurgeons have played such a central role in advancing neuroendovascular therapy in Japan. About 90% of members are neurosurgeons, while radiologists, internists, emergency physicians, and researchers also participate. In Europe and the United States, neuroradiologists initially pioneered and expanded this field. However, in recent years, even major countries have increasingly developed a structure similar to Japan’s, with neurosurgeons heavily involved. Meanwhile, due to the rapid increase in endovascular treatment for acute ischemic stroke and carotid stenosis, there has been a notable rise in participation from internists (neurologists and cardiologists) and emergency physicians, broadening the society’s scope further.

Board-Certified Specialist System
Board-certified neuroendovascular specialists certified by JSNET require basic certification from the Japan Neurosurgical Society, the Japan Radiological Society, the Japanese Society of Internal Medicine, or the Japanese Association for Acute Medicine. In 1997, a preparatory committee of six members was formed. In 2000, the specialist system was officially approved by the society, launched by 14 board members who served as supervising instructors. In 2001, 34 instructors were certified through the first review, and from 2002 onward, the board certification examinations were held. A board-certified neuroendovascular specialist is defined as “a physician who possesses broad knowledge and clinical experience in neuroendovascular therapy, including disease pathology, indications, treatment methods, and complications, and who has the technical ability to safely perform basic procedures independently.” This definition has been strictly maintained from inception to the present.
To qualify, candidates must have sufficient clinical experience, perform cerebral and spinal angiography as operators, and undergo specialized neuroendovascular training. The certification examination consists of written, oral, and practical components. Initially, live performance testing was required, but from the 5th exam (2005), the system shifted to on-site audits. In 2010, audits were waived for those trained at certified institutions with supervising instructors and a sufficient case volume, and by 2020 the system was abolished entirely. Because the examination includes a practical component, it is highly regarded as the best method to evaluate technical competence. Candidates must also complete a set number of angiographies and treatments at certified training facilities. Pass rates are not high compared to other specialties, ensuring quality control. By 2024, 2,428 specialists had been certified, and 286 certified training facilities were registered.
Supervising instructors can apply after obtaining specialist certification. They must demonstrate sufficient clinical experience, research, and academic activity (e.g., publications, conference presentations) and are approved after review. To date, 557 supervising instructors have been certified. Specialists are defined as those with excellent knowledge, skills, and clinical/educational ability, while supervising instructors must also fulfill leadership roles in research. Both certifications must be renewed every five years, requiring ongoing clinical practice.
Meanwhile, with the proven benefit of thrombectomy for acute ischemic stroke, a separate certification system for physicians focused exclusively on thrombectomy was introduced in 2020 by JSNET in collaboration with the Japan Neurosurgical Society and the Japan Stroke Society. JSNET manages the certification process, and as of 2024, 812 physicians were certified. The Japan Stroke Society requires that Primary Stroke Centers (PSC Core Facilities) have at least three full-time certified specialists and/or thrombectomy-certified physicians combined. This system has greatly improved patient transport and treatment efficiency in the acute stroke setting. (Figure 1)

Official Journal
From the society’s founding, the concept was to preserve academic records. The proceedings “Transactions of the Study Group of Intravascular Surgery” were published, serving as a bible at a time when information was scarce. To align with internationalization, in 1997, WFITN’s journal Interventional Neuroradiology was adopted as the official journal, and excellent Japanese papers were published as supplement issues in English.
Following incorporation as an NPO, the Japanese-language journal “Journal of Neuroendovascular Therapy (JNET)” was launched in 2007, published quarterly. In 2015, JNET became an English-language journal. However, due to strong demand, a Japanese-language journal “Neuroendovascular Therapy” was also maintained. From 2022, JNET was unified as an English journal, with no Japanese submissions accepted. As submissions increased, acceptance rates declined and quality rapidly improved. In 2023, JNET was indexed in literature search engines, and in 2024, it achieved PubMed listing and obtained an impact factor.
Thanks to the efforts of successive editors-in-chief—Masaki Komiyama, Ichiro Nakahara, Shinichi Yoshimura, and Ichiro Kiyosue—JNET has developed significantly. The journal is expected to grow further as a leading international publication.

Educational System

Training and fostering of neuroendovascular physicians were initially conducted only in the facilities of pioneering doctors, and one could learn techniques only through domestic and international conferences. In 1990, however, the first “Neuroendovascular Surgery Training Course” (held in Atami) was launched as a hands-on program. From then on, consensus on treatment techniques gradually emerged and was disseminated. Since the 18th annual meeting in 2002, Akio Hyodo, as chair, started the Continuing Education Program (CEP), which has since been held every year. Today, participation in CEP is required for specialist recertification.
Additionally, regional academic meetings are regularly held several times a year across seven regions, creating an at-home atmosphere where the latest information is shared and in-depth discussion nurtures young doctors. Supervising instructors also lead national educational seminars and live demonstrations. Regional and institutional groups actively hold morbidity and complication conferences. Furthermore, hands-on seminars organized by both industry and the society are conducted nationwide. In recent years, online lectures and expert training videos distributed via private streaming services and social media have made it easier for doctors to acquire knowledge and skills anytime and anywhere.
In 2007, when JSNET joined the Japanese Board of Medical Specialties, educational guidelines for neuroendovascular specialists were drafted under the leadership of President Kazuro Taki, with Nobuyuki Sakai and Shigeru Miyachi preparing the text, though it was not published. Later, in preparation for the new specialist system under the Japanese Medical Specialty Board, standards for the neuroendovascular training system were finalized by Masayuki Ezura and the committee. In November 2019, the board adopted the “Neuroendovascular Specialist Training Curriculum” and the “Training Logbook,” and from 2020, new residents were required to register as trainees and use the logbook.
As for textbooks, the first translation of a Russian endovascular surgery text was published in 1989. In the early years, the “Transactions of the Study Group of Intravascular Surgery” and society journals were virtually the only resources. Since the 21st century, however, numerous case-based textbooks and disease-specific manuals have been published, widely read, and very useful for lifelong education of members.

History of Neuroendovascular Therapy
1. Cerebral Angiography
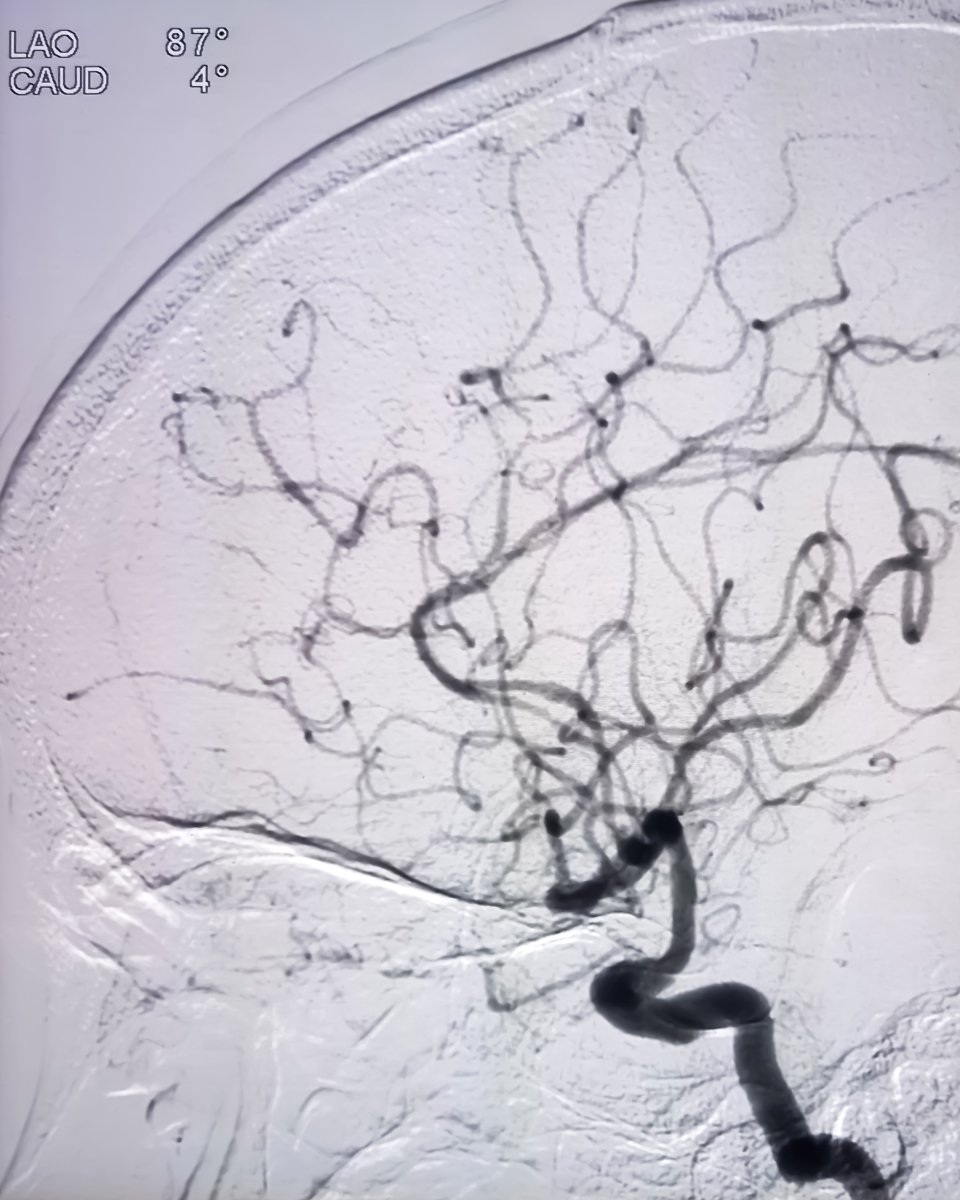
Neuroendovascular therapy is based on cerebral angiography. The history goes back to 1927, when Egas Moniz introduced cerebral angiography, and almost simultaneously in Japan, Professor Makoto Saito of Nagoya University developed the method. Soon after, venous catheterization was invented, and in 1941, Farinas devised the arterial catheter method. A major breakthrough came in 1953, when Seldinger introduced the percutaneous catheterization technique, which remains the foundation of all angiography and endovascular procedures today. Traditionally, access was via femoral artery puncture. Recently, however, the transradial approach—widely adopted in cardiology—has also become common in neuroendovascular procedures, reducing invasiveness for patients.
Initially, angiography involved serial film exposures, with subtraction performed manually by overlaying inverted pre-contrast films onto angiography films. Around 1990, Digital Subtraction Angiography (DSA) emerged, enabling real-time subtraction and greatly improving understanding of vascular structures. With rotational angiography, 3D-DSA was developed, allowing three-dimensional visualization. Today, high-resolution biplane systems, IVR-CT, and cone-beam CT are widely available, enabling multiperspective imaging. Phase changes can now be visualized in color, while nonionic contrast media have reduced vascular irritation and osmotic complications.
2. Evolution of Treatment Methods
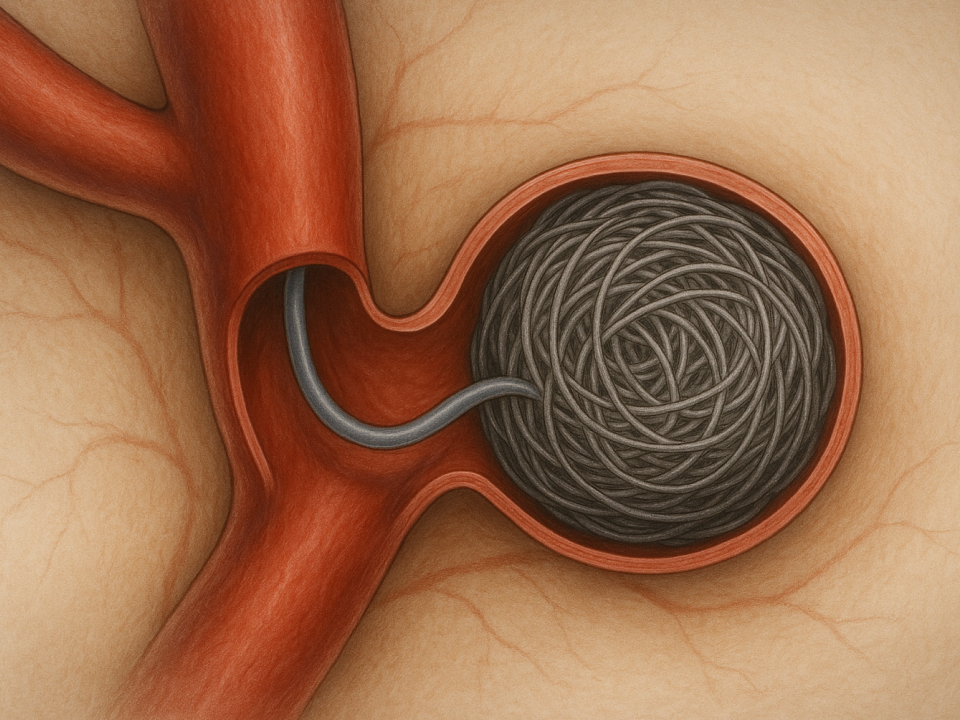
History of Embolization
The earliest report of head and neck embolization is thought to be in 1904, when Dawbarn injected paraffin and vaseline into the carotid artery to embolize vessels feeding a facial sarcoma.
In 1931, Brooks performed the first selective embolization by inserting a muscle fragment into a traumatic carotid-cavernous fistula. Although embolic materials at that time relied on blood flow for delivery, and selectivity was limited, the natural flow diversion in shunt lesions allowed reasonable accuracy. This principle is still applied today in flow-guided catheter techniques.
In Japan, the “leak balloon” developed by Taki and colleagues in the 1980s was widely used for cerebral arteriovenous malformations, applying a similar approach.